24 The rate of spontaneous vaginal delivery was no different between the two groups, although patients who immediately pushed had a shorter total second stage (−31.8 minutes 95% CI, −36.7 to −26.9), a longer duration of active pushing (9.2 minutes longer 95% CI, 5.8 to 12.6), less chorioamnionitis, and fewer postpartum hemorrhages. 23 However, a randomized controlled trial of 2,414 nulliparous patients with epidural anesthesia compared immediate pushing after complete cervical dilation with pushing after a 60-minute delay. It is also associated with a small increase in the rate of spontaneous vaginal delivery (risk ratio = 1.07 95% CI, 1.02 to 1.11). According to a Cochrane review, laboring down results in a longer (by 56 minutes) second stage of labor overall but a shorter duration of active pushing (by 19 minutes), compared with immediate pushing. This allows for spontaneous descent of the fetal head to a lower station, without pushing, after full cervical dilation is obtained. 34, 37Īmerican College of Obstetricians and Gynecologists guideline and Cochrane reviewĭelaying maternal pushing, also known as laboring down, is another approach to consider. 33Ĭonsider offering elective induction of labor to low-risk nulliparous patients at 39 weeks' gestation. 
One-on-one assistance from a trained labor support person (e.g., a doula) leads to improved outcomes. 3, 30Īmerican College of Obstetricians and Gynecologists guideline and small retrospective study Large retrospective study and Cochrane reviewĬonsider manual rotation of occiput posterior presentation it reduces rates of cesarean delivery and severe perineal lacerations. Use low-dose, rather than high-dose, oxytocin regimens when labor augmentation is required. Large cohort data and American College of Obstetricians and Gynecologists guidelines Cesarean delivery should be reserved for patients meeting criteria for arrest of labor and who have undergone an adequate attempt at labor augmentation including oxytocin (Pitocin) and amniotomy. Elective induction at 39 weeks' gestation in low-risk nulliparous patients may reduce the risk of cesarean delivery.Īrrest of labor should not be diagnosed before active labor begins (i.e., cervix is dilated to 6 cm). Effective measures for preventing dystocia and subsequent cesarean delivery include avoiding admission during latent labor, providing cervical ripening agents for induction in patients with an unfavorable cervix, encouraging the use of continuous labor support (e.g., a doula), walking or upright positioning in the first stage, and not diagnosing failed induction during the latent phase until oxytocin has been given for 12 to 18 hours after membrane rupture. When contractions or pushing is inadequate, vacuum or forceps delivery may be needed. Primary interventions for a protracted second stage include use of oxytocin and manual rotation if the fetus is in the occiput posterior position. This stage is considered protracted if it lasts three hours or more in nulliparous patients without an epidural or four hours or more in nulliparous patients with an epidural. The second stage of labor begins at complete cervical dilation and continues to delivery. Managing a protracted active phase includes oxytocin augmentation with or without amniotomy. 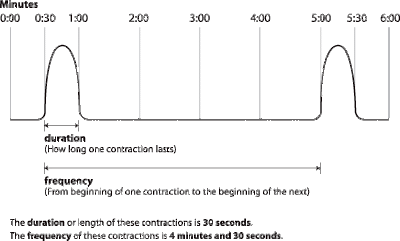
An arrested active phase is defined as more than four hours without cervical change despite rupture of membranes and adequate contractions and more than six hours of no cervical change without adequate contractions. Current recommendations are to avoid admission to labor and delivery during the latent phase, assuming maternal/fetal status is reassuring. The latent phase of labor begins with onset of regular, painful contractions and continues until 6 cm of cervical dilation. Dystocia (abnormally slow or protracted labor) accounts for 25% to 55% of primary cesarean deliveries.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
